Coming Full Circle: A Story of a NICU Nurse Turned NICU Mother
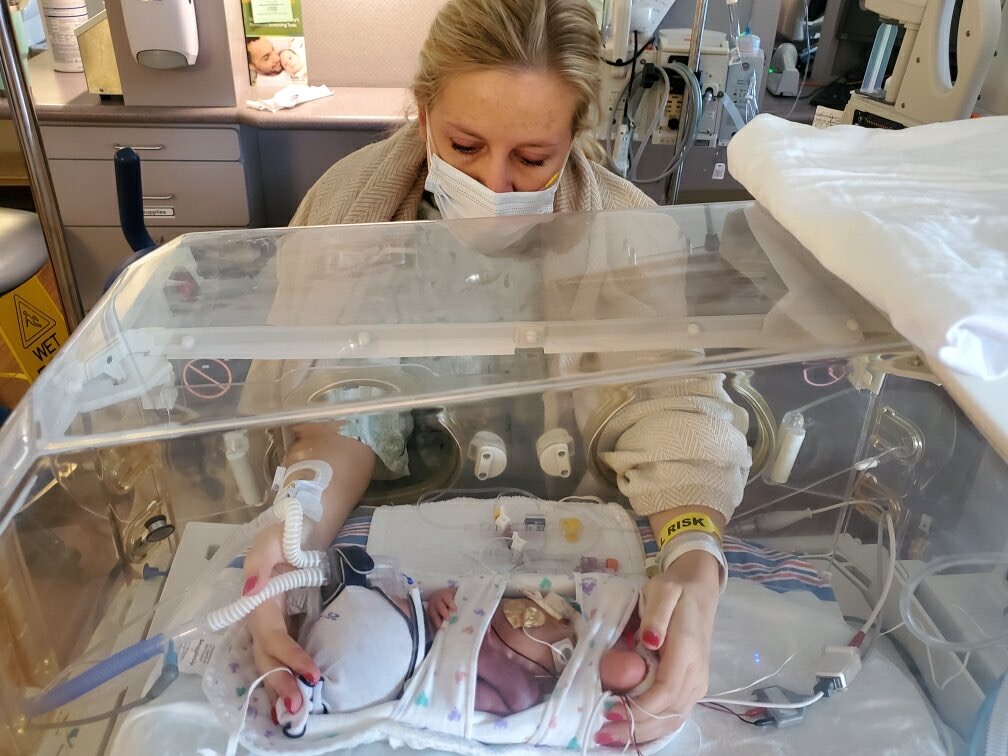
A very personal message from Amy Wiford BSN, RN, NTMNC. Amy is one of our valued clinical advisors, who is also a preemie mom.
 “I couldn’t work around sick babies. I don’t know how you do it.” The infamous statement every neonatal professional has heard. Like many NICU nurses, I was called to this field of nursing before having babies of my own. For many years, I dreamed of having a baby; although, the thought of carrying a baby for nine months was terrifying.
“I couldn’t work around sick babies. I don’t know how you do it.” The infamous statement every neonatal professional has heard. Like many NICU nurses, I was called to this field of nursing before having babies of my own. For many years, I dreamed of having a baby; although, the thought of carrying a baby for nine months was terrifying.
It was an absolute dream come true when I learned I was pregnant; that dream eventually turned into a real-life nightmare. As a NICU nurse, I thought through my baby’s weekly gestational development as he reached viability and slowly moved into the third trimester. Weeks shy of my third trimester, I was hospitalized with preterm labor at 26 weeks. I sat in my hospital room in disbelief that I was dilated and having contractions. I didn’t have a set labor plan, but I was certain this wasn’t my preference.
I vividly recall my consult with the NICU fellow while sitting in my sterile hospital room during my admission at 26 weeks. Her eyes grew larger and larger as I made my way through my lengthy, detailed, and pointed list of questions. Throughout our conversation, it became apparent to me that this facility had very different care practices and policies than what I had learned throughout my thirteen-year nursing career. I felt my entire world crash as I completely lost control of my pregnancy. My body continued contracting while I grew anxious about the quality of care my unborn son would receive. I’d never worked in the facility I was admitted to and wasn’t acquainted with the physical hospital environment or staff; their care practices and policies seemed foreign to me. Questions ran through my mind endlessly: Is this a safe facility? Will nursing staff care? Are they fully staffed? Do they have the necessary NICU equipment and protocols? Are my doctors top-notch? I felt vulnerable as I realized it was mid-June, and I was admitted to a teaching facility. I was comfortable and confident on the clinician side of the fence, and I wasn’t interested in finding out if the grass was greener on the parent side.
I was determined to stay pregnant and give my son time to grow and develop, but deep down I knew it was only a matter of time before he made his grand entrance. I’ve devoted my entire career to neonatal nursing, but nothing prepared me as I stood in line for the roller coaster ride that I had previously described to so many families.
I delivered my premature son at 28 weeks, which came with a wide range of intense emotions. When I first met my son, I had been a nurse for thirteen years and a mother for a few hours. Unlike other NICU parents, I was qualified to take care of my son. I had the knowledge and skill to care for him just as every other nurse in his NICU. I felt overwhelmingly helpless as I now sat on the lonely, unfamiliar parent side of the isolette. It was as if I was walking on eggshells with my hands tied behind my back, unable to silence his continuous alarms, adjust his CPAP headgear, wean his oxygen when he was high sating or feed him as he cued. Throughout his entire stay, I vacillated between making decisions and participating in his care as his nurse as opposed to his mother. I attended rounds nearly every day and intently listened as his providers discussed his daily plan of care. His team asked for my input each and every day, which consistently jolted me back to reality. They weren’t discussing my patient; they were discussing my son in the isolette beside me! My son’s unit ascribed to Family Integrated Care principles which was a highlight of his care, as it fueled my need for control and inclusion. My need for control didn’t completely subside, as I struggled with role alteration throughout most of his stay.
As the first few days went by, I became more comfortable with the staff and painfully adjusted to the “new normal” of being away from my son. Leaving him in the NICU with a care team full of strangers was the first of many hurdles I had to overcome. I spent six to eight hours at his bedside every day, which gave me the opportunity to bond with him as well as get to know his care team. I was sensitive not to overstep my motherly boundaries and become “that family” nurses dreaded caring for. It took me time to “learn” his nurses and vice versa. Over time he had a full primary nursing team that provided exceptional care to both my son and myself. His team of nurses took me under their wings and provided me with unconditional love and support through this unimaginable roller coaster ride that was complicated by a pandemic. These nurses served as my friends and family as I strictly adhered to quarantine guidelines throughout my pregnancy and Theo’s inpatient stay. Even though I’m a nurse, I was just as hopeless as every other parent in this situation. Nothing would have prepared me for the experience.
